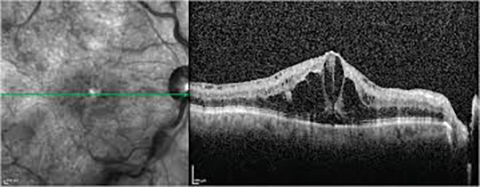
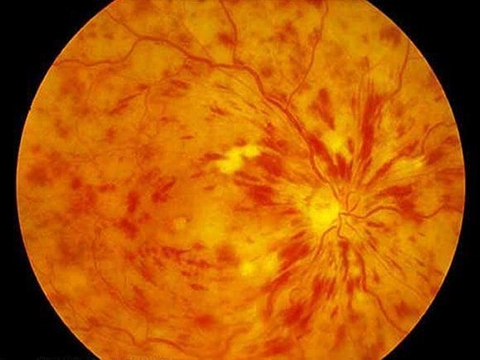
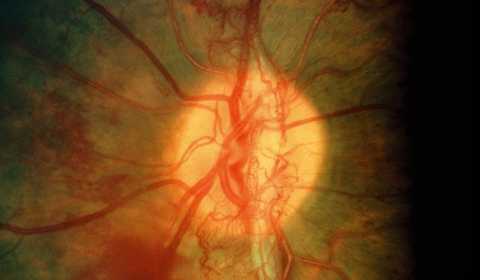
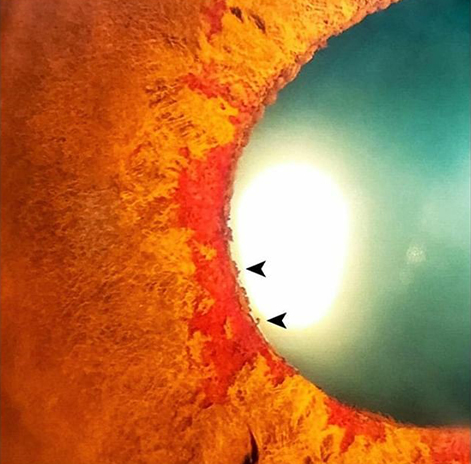
Treatment for the complications of retinal vein occlusion may include:
-
Focal laser treatment, if macular edema is present.
-
Injections of anti-vascular endothelial growth factor (anti-VEGF) drugs into the eye. The approved drugs are Lucentis, Eylea and Ozurdex.
-
Treatment of secondary glaucoma caused by growth of new blood vessels in the front compartment of the eye (neovascular glaucoma)
How are intravitreal injections performed?
An intravitreal injection is a shot of medicine into the eye. The inside of the eye is filled with a jelly-like fluid (vitreous). During this procedure, your health care provider injects medicine into the vitreous, near the retina at the back of the eye. The medicine can treat certain eye problems and help protect your vision. This method is most often used to get a higher level of medicine to the retina.
How many injections can I expect to need?
Most people who get anti-VEGF injections will need injections once a month for at least the first 3 months. Over time, you may need injections less often. On average, the first year is the most intensive period with most patients needing about 8 injections over 12 months.
I’m terrified of pain – how painful are injections into the eye?
Adequate numbing drops will be applied to ensure that the procedure is fast and painless. Typically, patients feel pressure, with little or no pain during the injection. You may also feel a slight burning sensation that is related to the antiseptic used to clean the surface of the eye. The entire process takes about 10 to 15 minutes.
What are the possible complications of the procedure?
- Infection in the eye or endophthalmitis
- Inflammation in the eye
- Bleeding into the vitreous gel (vitreous hemorrhage)
- Retinal detachment
- Sometimes there may be a small bleed or subconjunctival hemorrhage on the surface of the eye where the needle enters; this usually heals within a week.
- Temporary rise in eye pressure that usually returns to baseline in a few minutes. If excessively high, your doctor may perform a minor procedure called paracentesis to draw a small amount of fluid from the eye to relieve the pressure quickly.
What steps can I take to avoid infection after the procedure?
It is important to avoid rubbing the eye as the most common source of infection is from skin bacteria. You should also try to keep the eye as dry as possible especially when taking a shower. You should not swim for at least a week after injection. Besides these, you may return to normal activities after 1-2 days, including driving, reading, watching television and light exercise.
What should I look out for after the injection?
You might notice a few floaters or small bubbles appearing in the corner of your vision after the injection. These are normal and will disappear within 2-3 days.
However, you should contact your ophthalmologist if you experience signs and symptoms of complications, such as:
- Eye pain
- Decreased vision
- Seeing many floaters after the first day
- Increased sensitivity to light